Thursday, April 25, 2024
 47.0°,
Mostly Cloudy
47.0°,
Mostly Cloudy
Glen Cove Hospital’s Denyce LaVeglia, ‘a true Florence Nightingale’
Tough times require strength, which LaVeglia has
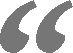
Keeping a promise is important to most 4-year-olds, and Mia Josephina Gambino is no different. It was difficult for her when she was separated from her parents, Joseph Gambino and Denyce LaVeglia, for three weeks when her father was diagnosed with Covid-19.
“Not seeing my daughter was the worst thing I could go through,” said LaVeglia, 36, a registered nurse and the assistant manager of Glen Cove Hospital’s rehabilitation unit. “You need that love and the feeling you get from your child, and I couldn’t have it. I wanted to run over and hug her, but I couldn’t. She began to shut down, and didn’t want to talk to me or my husband toward the end.”
Gambino, 38, began to show signs of the virus in the couple’s Dix Hills home in April, coughing and feeling fatigued. When he went to urgent care, he tested negative for Covid-19, but LaVeglia said she knew he had it. He began to decline quickly, experiencing shortness of breath, and three days later could barely breath. LaVeglia admitted her husband to GCH on April 15, and Mia was taken to LaVeglia’s parents’ house to protect her from getting sick.
Gambino improved within two days and was not put on a ventilator, but he remained in the hospital for a week.
“Denyce came to work even though her husband was sick,” said Evelyn Mulvaney, the assistant director of nursing at GCH. “Her little girl didn’t understand why she couldn’t play with her mommy. Denyce is such a great mom.”
The family reunited on May 2. “All three of us cried like big babies,” LaVeglia said. “But Mia still asks every day when I drop her off at my mother’s if she’s going to sleep there. When I first got her back and had to drop her off [there], she got so upset she wouldn’t let me leave. She kept making me promise that I’d come back.”
To make matters worse, LaVeglia said, her daughter’s need for hugs and kisses from her mother can’t be fulfilled. “I still have to social distance from her,” LaVeglia explained. “Mia wants to be affectionate, but I can’t be.”
LaVeglia was moved out of the rehabilitation department and became a hospital supervisor for six weeks when the coronavirus was at its peak. “It was a stressful time, because none of us knew what to expect and everyone was afraid of the unknown,” she said. “I had many interactions with patients and their families, which is a part of your everyday job as a nurse, but there were so many. People were dying. It was a sad reality.”
Covid-19 patients lose strength, Mulvaney said, and need encouragement to move around. “Denyce inspires people to work at getting better,” Mulvaney said. “I think she was the strength behind her husband getting better.”
LaVeglia is a compassionate caregiver, said Kim Rusnack, the rehabilitation department’s director of patient care services. It’s not uncommon to see her holding a patient’s hand while speaking to the family, and Rusnack said, she cares for her staff in much the same way. “During the beginning of Covid, Denyce was a big advocate of the staff making sure they had the proper [personal protective equipment] and that the units were stocked,” Rusnack recalled. “She is motherly of the staff, protective of them.”
A mentor of new hires, LaVeglia takes pride in knowing her staff. When a nurse’s mother died, LaVeglia took up a collection for flowers. She arranged for a baby shower for another nurse.
“Denyce epitomizes what a nurse should be,” Rusnack said. “She is a true Florence Nightingale. Patients and families love her.”
LaVeglia also sees the bigger picture, Rusnack said, by understanding the needs of the hospital as a whole.
Being a leader has its responsibilities, LaVeglia said. You have to have the utmost confidence, and be positive. A leader, she said, needs to carry on and keep spirits up when everyone else is down. “I remember one day we ran out of isolation gowns, and I could see everyone starting to panic,” she recounted. “I called them by name and asked them what was making them happy right now. It worked. They just needed to be brought up.”
With the number of Covid-19 cases dropping at GCH, LaVeglia is back in the rehabilitation unit. She is focused on helping patients who are still recovering grow strong enough to go home. The patients need a variety of help, including physical, occupational and speech therapy. “Either they were in the hospital so long on ventilators that their muscles start to decompensate, or they had a stroke and then got Covid,” she said. “They have to build up their strength. All of the patients I see are either post-Covid or still have it.”
Their ages vary from 23 to 90, she said, though most are between 60 and 70.
“Making someone smile makes you feel good during these times,” she said. “And it melts my heart when someone says something nice to me, giving me recognition like I got at Target recently. But this is what I do. I became a nurse to help people.”
HELP SUPPORT LOCAL JOURNALISM
The worldwide pandemic has threatened many of the businesses you rely on every day, but don’t let it take away your source for local news. Now more than ever, we need your help to ensure nothing but the best in hyperlocal community journalism comes straight to you. Consider supporting the Herald with a small donation. It can be a one-time, or a monthly contribution, to help ensure we’re here through this crisis. To donate or for more information, click here.
Sponsored content
Other items that may interest you







