Surgery saves life of Valley Stream Covid-19 patient

Valley Streamer Shirelle White survived Covid-19, but her road to recovery has been a long one. In early May, after returning home from receiving in-patient care at both Mather Hospital and Long Island Jewish Medical Center, White, 55, said she still felt like she was breathing through a straw.
“I was very scared and nervous . . . At times I felt like I couldn’t breathe at all,” she said. “Everyone should be afraid of Covid-19 . . . I’m lucky to be alive.”
White was admitted to the hospital on April 3, after testing positive for the coronavirus. A severe asthmatic, she was quickly placed on a ventilator because she could not breathe on her own, and at more than one point her kidneys failed, requiring her to be placed on dialysis three times a week.
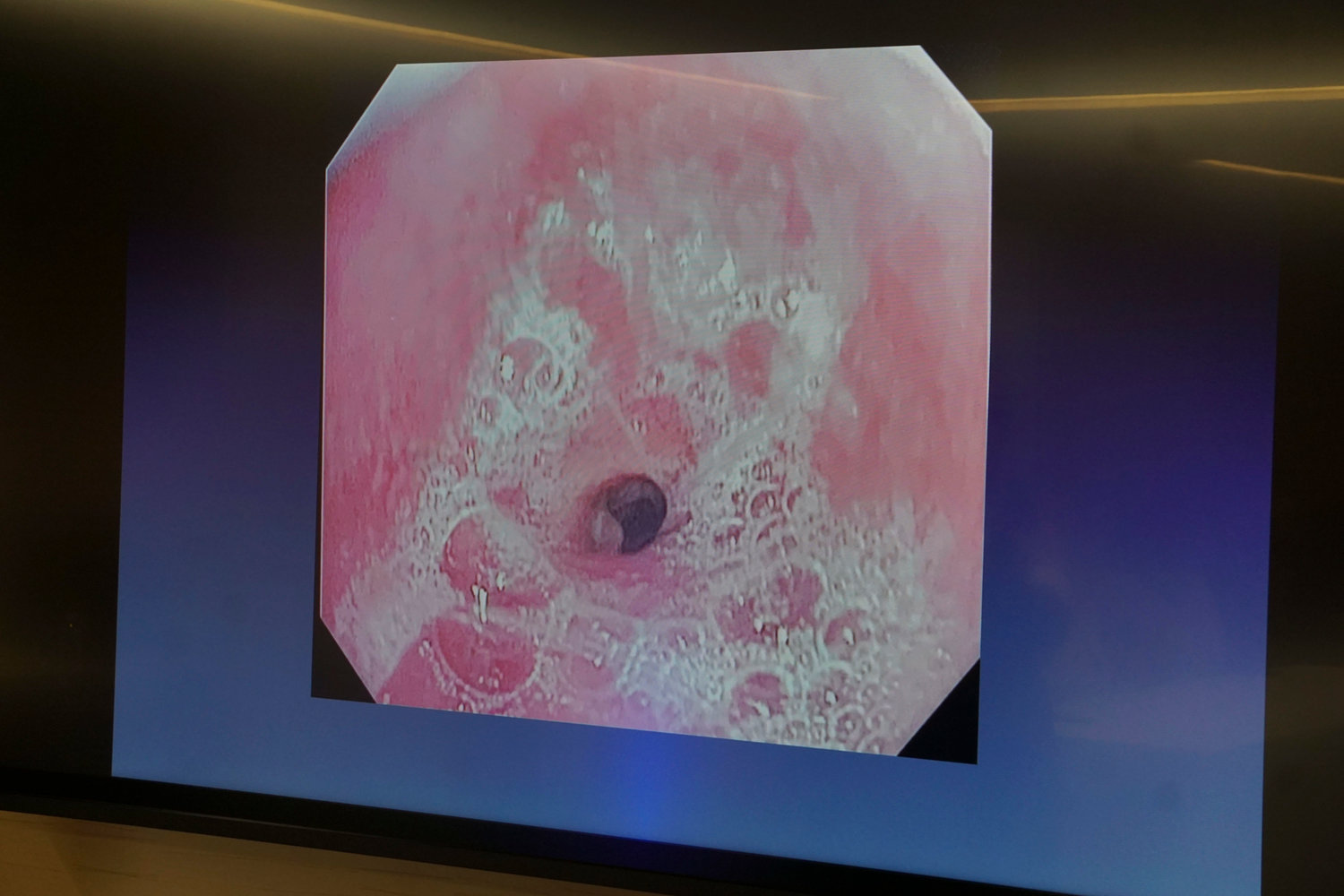
She improved, however, and on April 24, doctors took White off the ventilator. By May 8, she was home, but her breathing troubles returned. Doctors discovered that the ventilator tube had scarred her trachea, obstructing it and creating a condition called tracheal stenosis.
“We sent her for imaging studies to confirm the diagnosis that I was sure she had . . . It was tracheal stenosis, and that isn’t something treated with medication,” said Dr. Arthur Trust, White’s pulmonologist for many years. “She was very nervous when I told her she was going to need surgical treatment for it.”
Trust suggested that White seek treatment with Dr. David Zeltsman, who immediately performed a tracheal resection operation at Long Island Jewish Medical Center to remove the damaged section of White’s trachea; the two healthy ends of the trachea were then sewed together.
“There was not much air flow going into her lungs, and that was part of the problem,” Zeltsman said. “The second issue was that she couldn’t exhale as much under such circumstances.”
Zeltsman said he performs about a dozen tracheal resection operations a year on patients suffering from tracheal stenosis, but noted that it was so far a rare complication among Covid-19 patients.
“The trachea is very sensitive, so that’s why tracheal stenosis happens, but it isn’t common in Covid-19 patients,” Trust said.
Speaking in a raspy whisper after the operation, White said the procedure had vastly improved her breathing. She still requires oxygen from a machine, however.
“I went into surgery nervous, and when I woke up after surgery, it wasn’t as bad as I thought it would be, and I discovered I was able to breathe,” she said. “Recovery wasn’t as bad as I thought it was, and I was on my feet right after coming out of surgery. Without the help of Dr. Zeltsman and Dr. Trust, my breathing would not be as good as it is now, so I thank them.”
White also expressed gratitude to her partner of 20 years, Maggie Raabe, who is also a Covid-19 survivor and a registered nurse.
“I want to thank Northwell for bringing Shirelle to where she is today. She still needs assistance putting her T-shirts on and off, but she is strong-willed and determined, and she beat the odds,” Raabe said. “I’m thankful to God, the two doctors and to White for her determination. People need to wash hands, wear masks and social-distance because this is serious.”