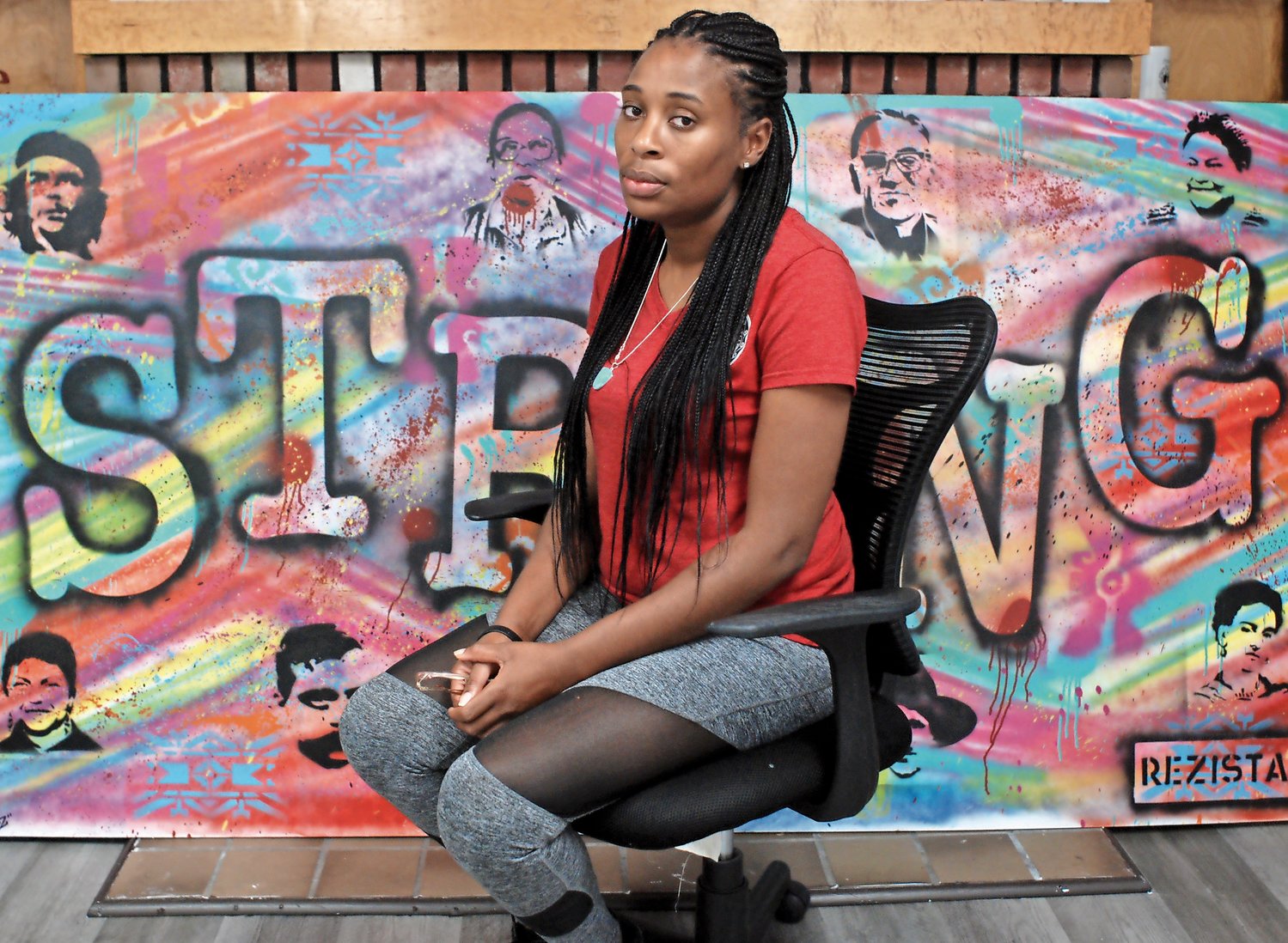A question of race and ‘birth justice’
Why babies of color are more likely to die in state’s second-healthiest county
Part one in a series.
When Sharelle Allen gave birth to her first child in 2014, the now 31-year-old wanted a natural experience — no monitors, no pain medication, no epidural, no C-section. Those were her rules.
“I wanted to be just free,” the mother of two said. “I wanted to eat and drink. I wanted to breastfeed.” She was in labor 44 hours — six in active labor.
When she gave birth the second time three years later, the experience was very different. Labor came on suddenly, in what is known as a “precipitous birth.”
“I was experiencing a lot of pain,” she said recently at STRONG Youth, the Uniondale-based nonprofit gang-prevention and community-development organization where she is the lead intervention case manager. “It was very abrupt on my system. I was screaming for pain medication.”
No one answered, she said. During birth, she suffered a vaginal tear and received four stitches without pain medication. Twelve hours later, Allen said, she was given the pain reliever she had begged for during the birth.
Her experience — the sense that no one was listening and responding to her concerns — led Allen, who is African-American, to join Birth Justice Warriors, a growing group of two dozen black and brown women who are working to raise awareness of the wide disparities in maternal care received by women of color and white women.
Dr. Martine Hackett and Dr. Nellie Taylor-Walthrust, both women of color, started the group in March 2018. Hackett is an associate professor of health professions at Hofstra University, and Taylor-Walthrust, a pastor, is director of outreach services for the North Shore Child Family Guidance Center, a nonprofit mental health agency with offices in Roslyn Heights, Manhasset and Westbury. They get the word out through small group discussions and community forums.
The objective, Allen said, is to “build a community of concern so we know what our rights are, so we can birth the way we want to in the most healthy way.”
When infants die
Among the central issues that Birth Justice Warriors is working to address is infant mortality, which is a leading indicator of a community’s well-being, according to the Nassau County Department of Health’s 2016-18 Community Health Assessment and Community Health Improvement Plan. When children are dying in high numbers at birth — the start of life — there are probably myriad other health concerns in a community.
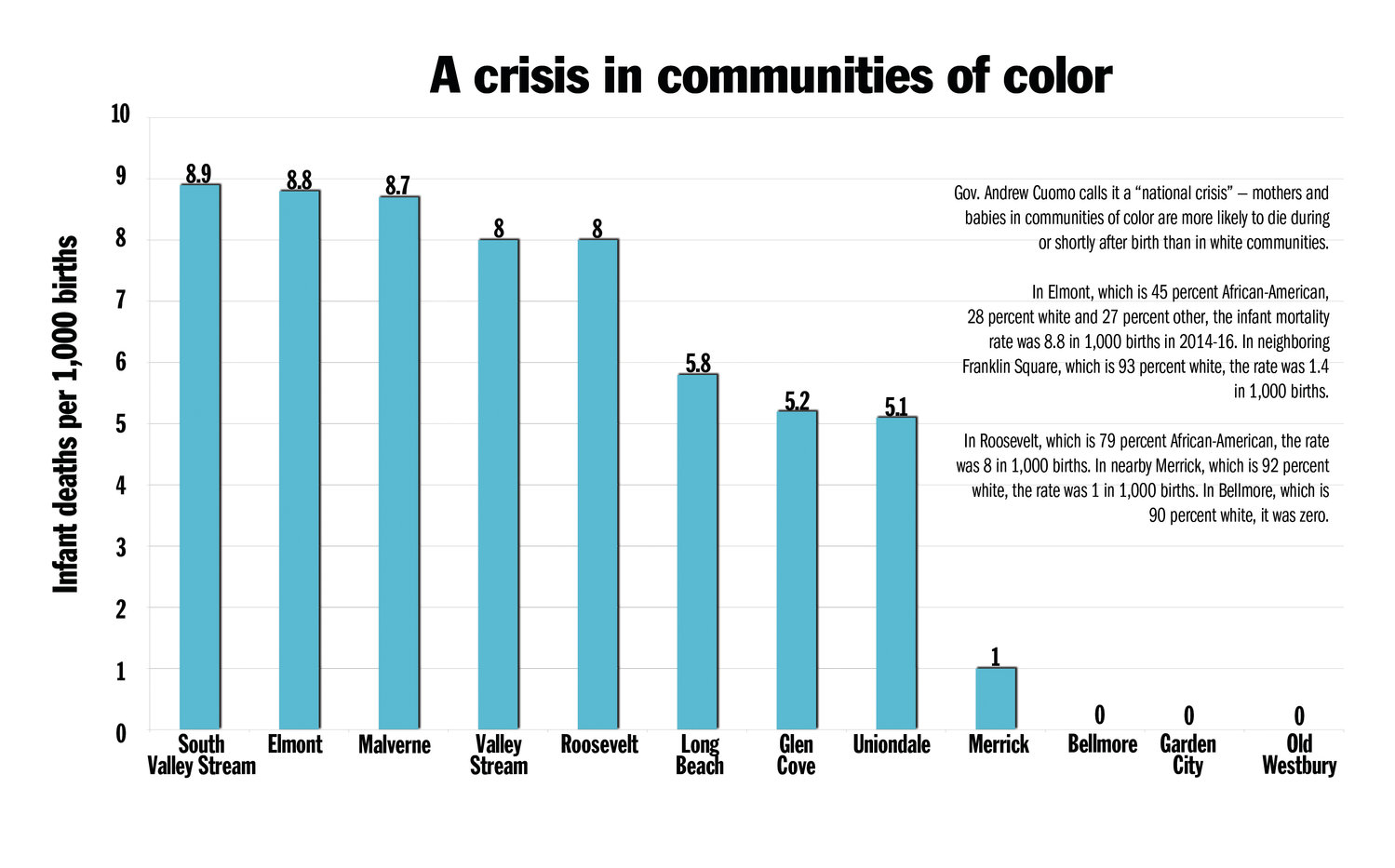
In the majority of white communities across Nassau, the infant mortality rate ranged from 0 to 3 in 1,000 births in 2014-16, according to the New York State Department of Health. Meanwhile, in most communities of color, the infant mortality rate was three to nine times that.
In its annual rankings of healthiest counties in New York, the Robert Wood Johnson Foundation, working with data from the federal Centers for Disease Control and Prevention, ranked Nassau the second-healthiest of 62 counties in the state this year. When that data is broken down into individual zip codes, however, a disturbing pattern is made clear in communities of color, Hackett said: Babies there are significantly more likely to die during or shortly after birth than in predominately white communities.
When “looked at as the aggregate,” she said, the county’s “health outcomes are great.” That, she said, “creates this illusion that everything is fine here.”
But, she added, “there are health conditions that are worse here in Nassau County than New York City.”
Three calls to the county health department were not returned. Its own 2016-18 assessment, however, supports Hackett’s assertion that there is a wide gap in health outcomes between communities of color and white communities locally.
County officials identified nine communities of color and communities with large minority populations — Elmont, Freeport, Glen Cove, Hempstead, Inwood, Long Beach, Roosevelt, Uniondale and Westbury — each with measurably greater health concerns than nearby white communities.
Nassau is the 13th-wealthiest county in the U.S., with an average annual household income of around $93,000, according to census data. “The affluence of the county as a whole masks the needs of these severely underserved selected communities,” the county’s report states.
Taken as a whole, the infant mortality rate in these communities is “nearly double that of the rest of the county,” the report continues.
The knee-jerk reaction to explain the discrepancy is to blame it on a discrete factor like income level, according to Hackett: Women with fewer financial resources are unable to afford the same level of care that women of greater means can. But statistics tell a more complicated story.
How, for example, does one explain Elmont, a solidly middle-class community of color with an annual average household income of $94,353, slightly above the county average? It has the second-highest infant mortality rate in Nassau.
Access to health care alone “is not sufficient” to explain the disparities in health outcomes, Hackett said. Bias and systemic racism also play their parts, she believes.
Implicit bias
Among many subjects, Hackett studies “implicit bias” in her research — assumptions that people make about others, particularly those who are perceived as different. Implicit bias “doesn’t just live in our brains,” Hackett said. “It presents in our day-to-day actions.”
Implicit bias, she said, is why a white police officer might be more likely to pull over a person of color for a possible traffic violation — or why a white doctor, nurse or midwife might be more likely to ignore the insistent pleas of a woman of color enduring birth pangs.
There is a long-held belief in the medical community, spoken and unspoken, that African-Americans have a higher tolerance for pain than white people, Hackett said, and so black people are less likely to receive pain relief, even when they demand it.
African-American women, Allen said, are accustomed to being ignored. “It’s the way I walk through life,” she said. “My voice doesn’t matter.”
That black women’s concerns are often overlooked, even when voiced vehemently, helps explain why maternal health outcomes in many communities of color are significantly worse than in white communities, according to Hackett.
She was careful to note that there are several reasons for the discrepancy in outcomes, but implicit bias, even racism, in the medical community is among them.
“It has to do with the way women are treated — black people are treated — in the clinical setting,” she said.
The role of ‘microaggressions’
Te-Ana Souffrant, 36, who is African-American, is another member of Birth Justice Warriors. She grew up in an upper-middle-class family. She earned a master’s degree in health administration from Hofstra. She lives in affluent Baldwin Harbor. She is, by profession, a doula, a woman, usually without obstetric training, who provides guidance and support to pregnant women, even in the delivery room.
Souffrant, a mother of three, said that medical professionals often demonstrate their biases through “microaggressions,” seemingly small quips with much larger racial implications. When offering her and her husband a test for sexually transmitted diseases during one of her pregnancies, a doctor “joked” that “you better hope the result is negative . . . You better hope nothing comes back,” she said. Souffrant and her husband, a New York City corrections officer, were shocked. She was taken aback that a doctor would offer the test to a long-married couple, and she saw deeper racial implications in the so-called jest.
“There’s an assumption about black women having multiple husbands,” she said. The doctor, she added, “thought she was being funny in that moment,” but, Souffrant noted, “I know that she has never said that to a white client.”
“You’re already dealing with stressors as a black or brown person in this country that white people can’t even understand, on a daily basis,” she said. “I’ve had doctors who have made me feel less than.”
Because women of color are often made to feel that way, Souffrant said, there is “mistrust between black people and the medical community.” Distrust, in turn, leads many women of color to “not seek care” when they need it.
“There are multiple things happening all at once,” she said. “The root of it is racism.”
Chronic stress
At the same time, Hackett said, many women of color live in segregated neighborhoods. Schools in such communities are perennially underfunded. Crime rates may be higher. Family incomes are lower, so affording life’s necessities is harder, particularly in an expensive county like Nassau, where the cost of living is 1.5 times higher than the state average.
“Conditions of structural racism have an effect on individual bodies,” Hackett said. The daily stress that many women of color must live with, she said, “has a physical manifestation” that, in part, explains the discrepancies in infant mortality rates.
A 2017 study by the National Academy of Sciences, Engineering and Medicine, “Communities in Action: Pathways to Health Equity,” backs Hackett’s assertion.
“The impact of structural inequities follows individuals ‘from womb to tomb,’” the 558-page study states. “African-American women are more likely to give birth to low-birth-weight infants, and their newborns experience higher infant death rates that are not associated with any biological differences, even after accounting for socioeconomic factors.”
Changing the narrative
On Aug. 1, Gov. Andrew Cuomo signed legislation to create a Maternal Mortality Review Board, tasked with analyzing the reasons for the alarming discrepancy in maternal mortality between communities of color and white communities. “Racial disparities in maternal mortality is a national crisis,” Cuomo said at the bill signing, “and with the creation of this expert review board and advisory council, we are tackling the problem head-on.”
The 15-member board will comprise experts from the state and New York City departments of health, and doctors, nurses and health professionals. State Assemblywoman Michaelle Solages, a Democrat from Elmont, who is Haitian-American, championed the bill to form the board.
The board, she said, must address critical questions: Why are women of color “not getting access to prenatal care? Why are they not getting good nutrition? How can we combat implicit bias?”
“Why are a baby and a mother in Elmont more likely to die than in Garden City?” asked Solages, a 34-year-old mother of two. “It’s a huge difference . . . These are communities that are within a mile of each other.
“We really need to ensure that we’re getting the information out there that women can receive the support they need,” she continued. “We really need to talk about what’s going on in our community.”
“Hopefully,” Allen said, “we create a culture where it’s not birth justice. This is just the way we birth.”