Friday, April 26, 2024
 39.0°,
Fair
39.0°,
Fair
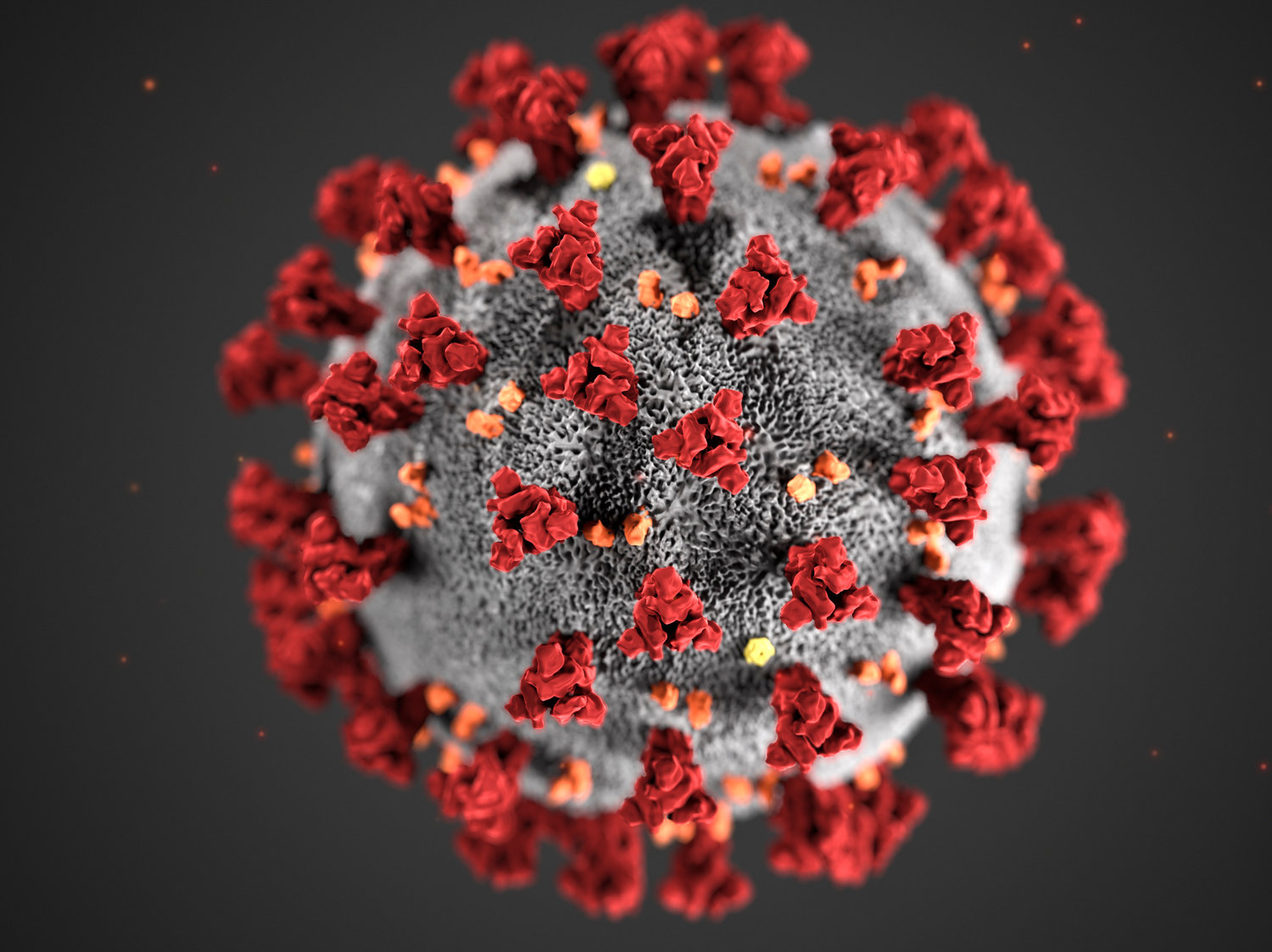
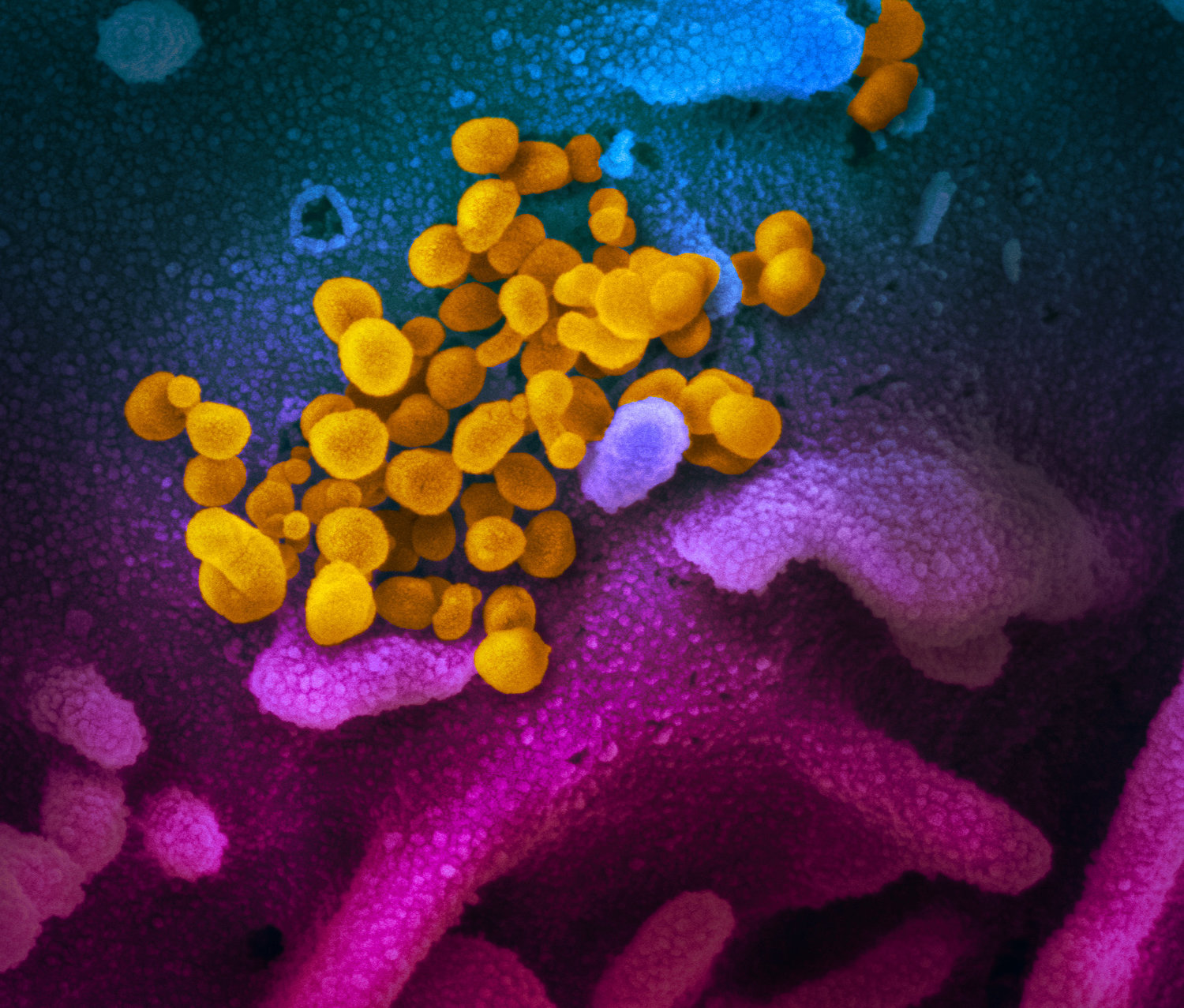
Glen Cove Hospital prepares for coronavirus
CDC says COVID-19 not a pandemic — yet
Coronaviruses typically affect the respiratory tract, with symptoms similar to the common cold and pneumonia. According to Tedros Adhanom Ghebreyesus, director general of the World Health Organization, COVID-19 is not as deadly as other types of coronavirus, including severe acute respiratory syndrome — SARS — or middle eastern respiratory syndrome — MERS. Eighty percent of patients with COVID-19 will recover, Ghebreyesus said at a press briefing on Monday. And there are few cases of infection among children.
“In about 14 percent of cases, the virus causes severe disease, including pneumonia and shortness of breath,” Ghebreyesus said. “And about 5 percent of patients have critical disease, including respiratory failure, septic shock and multi-organ failure. In 2 percent of reported cases the virus is fatal, and the risk of death increases the older you are.”
There is no vaccine to prevent coronavirus.
The Centers for Disease Control and Prevention is monitoring the number of people who may be infected with the coronavirus in the U.S. As of Feb. 17, these were the totals:
Tested positive for coronavirus: 15
Tested negative: 392
Pending: 60
Total: 467
States with confirmed cases: Arizona, California, Idaho, Massachusetts, Texas, Washington, Wisconsin.
Source: Centers for Disease Control and Prevention
As of Feb. 17, China had reported 70,635 cases of coronavirus, including 1,772 deaths.
That day, China reported 2,051 new cases.
94 percent of new cases continue to come from Hubei province.
Outside China, the World Health Organization had received reports of 694 cases in 25 countries, and three deaths.
Source: World Health Organization
Avoid close contact with people who are sick.
Avoid touching your eyes, nose and mouth.
Stay home when you are sick.
Cover your cough or sneeze with a tissue, then throw the tissue in the trash.
Clean and disinfect frequently touched objects and surfaces using a regular household cleaning spray or wipe.
Wash your hands often with soap and water for at least 20 seconds, especially after going to the bathroom, before eating and after blowing your nose, coughing or sneezing. If soap and water are not readily available, use a hand sanitizer that is at least 60 percent alcohol.
The novel coronavirus, dubbed COVID-19 by the World Health Organization on Feb. 11, had infected more than 70,600 people in China and killed more than 1,770 as of Monday, according to the WHO. The Chinese government built two hospitals in 10 days this month, an indication that the medical crisis would continue.
Although there were no reported cases in New York as the Herald-Gazette went to press, 15 people across the U.S. had been infected, prompting medical facilities, including Glen Cove Hospital, to prepare for the appearance of COVID-19 on the North Shore.
Northwell Health has plans in place for all 23 of its hospitals, including Glen Cove, if people become infected with the coronavirus. Mary Mahoney, Northwell’s vice president of emergency management and clinical preparedness, said that it would increase its isolation capacities in every hospital.
“We thought through what it would take if we had to add an additional 50, 100 or more isolation patients in our hospitals,” Mahoney said. “While this disease does not require a specialized treatment unit, the CDC does require private rooms,” she added, referring to the Centers for Disease Control and Prevention. “We would have 30 beds available at Glen Cove Hospital, the equivalent of two hospital wings.”
A specialized treatment unit was created on the third floor of the hospital during the Ebola outbreak in 2015, but was never used. Dr. Barbara Keber, the hospital’s chair of family medicine and Northwell’s vice chair of family medicine, agreed with Mahoney that patients with COVID-19 wouldn’t fit the criteria to use the treatment unit, and that the rest of the floor would be used instead.
Three patients from Glen Cove’s emergency room recently were concerned that they might have been exposed to the coronavirus, Keber said, but none had it. The hospital has a test kit for the virus from the CDC, but Keber said that no patients have qualified to be tested.
“We think COVID-19 is being spread by droplets, but this is all such a new thing,” she said. “The CDC isn’t calling it a pandemic yet. But we don’t have all the answers yet, which I think is making people nervous.”
People are more likely to have the flu, Keber said, or a respiratory virus, which has flulike symptoms. She recommends that people keep all surfaces clean, cough or sneeze into a tissue, which should then be disposed of, and stay home if sick. “We’ve sent some of our doctors home because they were sick,” she said. “People should avoid contact with people who are sick and avoid touching their eyes, nose and mouth.”
Why so many are infected in China
China’s outdoor markets include live animals that are butchered at customers’ requests. Similar to the swine flu, where the virus originated in pigs before humans contacted it, a virus can jump from one species to another.
“It was originally reported that the animal responsible was local, and now it’s believed to be pangolins that spread COVID-19,” said Dr. Mark Jarrett, Northwell’s chief quality officer and deputy chief medical officer. Pangolins, sold in outdoor markets, are popular in Asia, where their meat is considered a delicacy. “The pangolin may be the intermediary between bats and humans,” Jarrett explained, “with bats giving the virus to the pangolins. There is talk in China of maybe clamping down on having open markets.”
The effectiveness of wearing a mask
Many photos of people in China show them wearing masks. Jarrett said he didn’t blame them for trying to protect themselves, but masks aren’t that effective against the virus. The edges aren’t sealed, he said, and people aren’t being properly fitted for them.
Hospitals have always used masks — referred to as respirators — for airborne diseases like tuberculosis, Jarrett said. “We undergo fit testing so [the mask] fits properly,” he said. “Certain brands fit people better than others. Because of the tighter weave of these masks, people with breathing problems may have difficulty wearing it, and people that have beards can’t wear them at all.”
Jarrett said he didn’tbelieve it was necessary to wear masks in the U.S., and that it would be more effective to stand at least six feet from people who might be infected with the virus.
“We don’t know if COVID-19 will be a seasonal virus,” he said. “The flu generally goes away after the winter, but we just don’t know if that will happen with this virus.”
HELP SUPPORT LOCAL JOURNALISM
The worldwide pandemic has threatened many of the businesses you rely on every day, but don’t let it take away your source for local news. Now more than ever, we need your help to ensure nothing but the best in hyperlocal community journalism comes straight to you. Consider supporting the Herald with a small donation. It can be a one-time, or a monthly contribution, to help ensure we’re here through this crisis. To donate or for more information, click here.
Sponsored content
Other items that may interest you